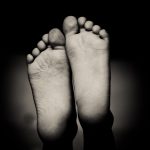
You may have noticed a little “bump” on the side of your foot, just to the side of your big toe. The bump that you see is actually the top, or head of the long metatarsal bone of your foot.
A bunion is medically known as HAV or Hallux Abducto Valgus. A bunion occurs when there is an abnormal protrusion of the first metatarsal head on the medial side, or the inside of the foot; it is also when the big toe moves laterally, or pushes up against the 2nd toe.
As the bunion progresses, the soft tissues around the metatarsal head (the bump) get inflamed and enlarge. This can cause more pressure on the bunion while wearing shoes, and can lead to more pain, and worsening of the bunion. Bunions are progressive deformities by nature. This means that they get worse over time. Bunions do not get better on their own. Various types of shoe gear, and physical activity can aggravate the bunion and make it worse.
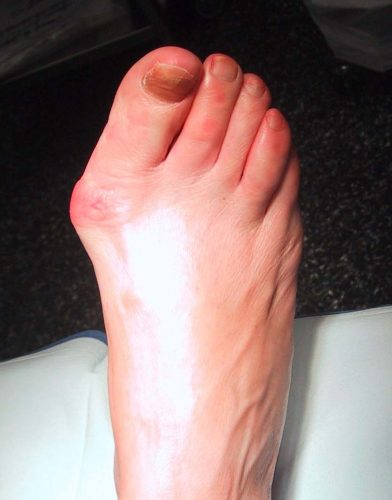
Etiology of the Bunion
Bunions are partially an inherited deformity. The structure of the foot is the genetic component, however environment and physical activity of each individual as well as the type shoes worn, can also affect how a bunion develops. Some bunions can develop at a very young age and are called Juvenile Bunions. However, bunions can also develop due to arthritis (i.e. Rheumatoid Arthritis).
Treatment of Bunions
There are two approaches to the treatment of bunions; conservative and surgical. Depending on the severity of the bunion and the type of bunion that a person has, conservative treatments can help to slow down the progression of the bunion deformity, and can also alleviate the pain associated with a bunion.
Conservative Treatments
- Shoe gear: Wearing the right shoes (i.e. shoes that are wide enough and do not put pressure on the bunion) is important. If the bunion is severe, then having a wide “toe box”, or space in the shoe where the toes will normally sit, is key. The shoes should also have a low heel, and have enough arch support.
An orthotic (custom made, or pre-fabricated orthotic or insert in your shoe) can also be used to help with increased arch support. It is essential for the shoes to have a snug fit at the heel. This helps to ground the foot. A heel that is not snug in a shoe will put added pressure on the bunions. - Padding: A gel or silicone padding that can fit around the big toe and protect the toe from rubbing against the side of the shoe is sometimes used to decrease the pain from the bunion. A gel padding that also has a silicone or gel spacer that separates the big toe and the 2nd toe will provide added protection and help to slow the progression of the bunion deformity.
- Bunion splints: Night splints for bunions have been shown to decrease the progression of a bunion. There are various types of splints, however they all aim to create space between the big toe and the 2nd toe, so that the big toe remains straight. Some examples are the “bunion bootie”, made of nylon and polyurethane which covers the big toe and stretches over the foot like a sock.
There are also bunion sleeves, or bunion correctors, that also have a sleeve that goes over the big toe, and stretches over the midfoot. - NSAIDs: Non-Steroidal Anti-Inflammatory medications in pill form can help to decrease the inflammation from a bunion.
- Steroid Injections: A steroid injection directly placed into the 1st Metatarsophalangeal Joint, or Big Toe Joint can temporarily alleviate the bunion pain and decrease the inflammation. An injection is used in cases where there is exquisite pain at the bunion.
- Physical Therapy: For bunions that are very painful, and are visibly inflamed; red, hot or warm to the touch, and swollen, therapy can alleviate the pain and calm down the inflammation. Light therapy, Ultrasound, and NSAID creams can be used as part of the physical therapy treatment regimen. Light massage with NSAID cream will decrease the inflammation of the bunion; however, massage alone will not effectively treat the bunion deformity.
Bunions that are not as severe can be treated more conservatively and these conservative treatments have helped. Some people will experience great relief for many months or years, and some people will need to use these conservative treatments off and on for extended periods of time.
Surgical Treatments
The second approach to the treatment of bunions is the surgical approach. Surgery can range from minimally invasive surgery (MIS) to an open incision surgery, called traditional bunion surgery (TBS). Essentially, there are four types of bunion surgeries, which can all be done with both minimally invasive surgery or traditional bunion surgery.
There is no non-invasive bunion surgery, as surgery is definitionally invasive.
Types of Bunion Surgeries:
- Exostectomy: This is the removal of the “bump” that is typically seen with a bunion deformity. This bump is the head of the long 1st Metatarsal.
- Osteotomy: Cutting the bone to realign the joint (1st Metatarsophalangeal Joint or Big Toe Joint). This may involve loosening of tight ligaments or tendons as well.
- Arthrodesis: Fusing a joint, especially if the joint is severely damaged, due to arthritis or physical microtrauma of the joint.
- Arthroplasty: Removing a part of the joint itself. This is also done for extremely damaged joints, especially with arthritis (Rheumatoid Arthritis), or with patients who have had previous unsuccessful bunion surgery.
Minimally Invasive Bunion Surgery (MIS) is where the incision made while performing surgery to correct the bunion is only 5-10mm long. The keyhole bunion surgery (done in the UK) uses several 3mm long incisions. Through this small incision, the surgery is done. Soft tissues are also released as part of the surgery. One type of MIS is called “keyhole bunion surgery” since the incision is as small as a keyhole. Because of the small incision, the healing process, in general, is typically much quicker than the traditional bunion surgery.
Scarring is minimized, there is less swelling after surgery, and there is a lower chance of a post-operative infection. As a result, there is also less pain after the surgery, and the patient can start walking much quicker as compared with a patient who underwent traditional bunion surgery. Most bunions can be corrected using MIS.
Traditional Bunion Surgery (TBS) involves a much larger incision, and the surgeon gains more visibility of the affected bunion in order to perform the surgery. This type of surgery may also be needed for more severe, and complicated bunions. A large incision may be needed if the bunion needs to be corrected using screws, plates or wires.
The TBS will take a longer recovery period. There will be increased swelling, redness, and a greater possibility of an infection. Depending on the hardware used, (Pins, Plates, Screws), and the type of surgery being done, the patient will need to remain off weight bearing until the bones heal completely.
Most insurances will cover MIS or TBS; a typical bunion surgery costs between 3000 -5000 dollars, depending on the location you are in, and the type of bunion surgery being done. In Ontario, Canada, most bunion surgeries are covered by OHIP (Ontario Health Insurance Plan)
Intra-Operative:
During surgery, if you are undergoing MIS, or Traditional Bunion Surgery, most doctors will only give the patient IV sedation with Monitored Anesthesia Care. You may be able to hear everything around you, but you will not be completely out as with General anesthesia.
Only the more severe bunion surgeries will need General anesthesia.
Post-Operative:
After the surgery is all done you can either walk right out of the operating room, or you may need to be completely off weight bearing for several weeks. With MIS, you will be able to walk much faster than with TBS. Healing of the bunion and soft tissues with MIS will take between 2-4 weeks; Traditional Surgery will take longer to heal, between 2-8 weeks.
In recent years, Minimally Invasive Surgery has gained popularity, due to the many advantages for the patient and doctor alike. There is a steep learning curve for MIS surgery, and today, Traditional Bunion Surgery is still done by most doctors. With the demand for MIS on the rise, more and more doctors will be pressed to learn the MIS techniques and to implement it in their practices on a regular basis.

Dr. Sharon Joag, DPM is a Podiatrist in Old Bridge, NJ and has been practicing for 14 years. She graduated from the New York College Of Podiatric Medicine in 2002, and had 3 years of surgical training at Metropolitan Hospital, Lincoln Hospital and Passaic Beth Israel Hospitals in New York and New Jersey.